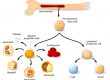
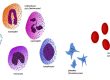
ET is a rare blood cancer which causes the body to produce too many platelets.
What is essential thrombocythaemia?
Patients with essential thrombocythaemia (ET) have an elevated platelet count; their blood contains too many platelets. The high number of platelets causes blood to be ‘‘sticky’’, so people with ET have a high risk of clotting or have bleeding problems because their platelets do not always work well. Sometimes the white cell count can be high in ET and this may also be important in blood clotting. However, some people with ET don’t experience any symptoms at all.
People generally develop ET as adults. Most people who develop ET are diagnosed at age sixty or older, but it appears that the blood cancer is becoming more common in younger people, especially women under forty.
Recent research has shown that about 50-60% of patients have a mutation (or change) in a protein called JAK2. 25-30% have a mutation in a gene called Calreticulin and another 2-5% of patients have a mutation in a protein called MPL. Both JAK2 and MPL are proteins which regulate blood cell production. Calreticulin is involved in calcium flow within the cell which is also important in growth signals. Researchers don’t currently understand what causes these mutations to occur.
Names for this disorder
Essential thrombocythaemia (ET) is sometimes called essential thrombocytosis or primary thrombocytosis (PT).
How common is ET?
ET is considered to be a rare blood cancer. The number of people diagnosed each year with ET will be between 1.5 and three cases per 100,000 and it is more common in women than men with two women diagnosed for every man.
Diagnosis
You might have visited your doctor to ask about symptoms, or your doctor may have discovered a high platelet count when you had a routine blood test. Your doctor will run diagnostic tests to determine whether you have ET or some other condition these are likely to be done through a specialist clinic run by a haematologist or blood doctor.
Reasons your platelets may be high
It’s possible for conditions other than ET to cause a high platelet count. Your haematologist will need to rule out any other possible underlying causes before making a diagnosis. Some conditions that increase the platelet count include:
- Infection
- Inflammatory disorders, for example arthritis
- Acute or chronic blood loss
- Tissue damage from trauma or surgery
- Splenectomy (removal of the spleen) or hyposplenism (when the spleen stops working)
- Some other blood conditions can cause a high platelet count
Signs and symptoms
Many people with ET do not feel any symptoms at all. Others may experience symptoms such as:
- Heart attack or stroke
- Persistent or repeated headaches
- Bruising and bleeding, including nosebleeds or heavy periods
- Burning pain, redness in hands or feet
- Gastrointestinal bleeding or blood in the urine
- Bleeding from nose or gums
- Dizziness or ringing in ears
- Itching or other unusual skin sensations
- Leg pains
- Coldness or blueness of fingers or toes
- Vision disturbances or silent migraines
Diagnostic tests
If your haematologist suspects you have ET, he or she may suggest some of the following tests:
- Full blood count (blood test): The full blood count or FBC shows how many cells are circulating in your bloodstream. Your haematologist will check your platelet count in particular. Platelets are the cells that help your blood to clot, and if you have ET, your bone marrow may be producing too many of these cells. A normal platelet count is 150 to 450 –– counts above 450 are considered higher than normal.
- JAK2 Calreticulin or MPL mutation test: Your haematologist can test your blood to see if you have a gene change (or mutation) called JAK2 V617F mutation. About 50% of people with ET show this mutation. 25-30% have a change in calreticulin and a small percentage of patients (2-5%) show a change in the MPL protein.
- Chest x-ray: You may need a chest x-ray.
- Abdominal ultrasound: If you have ET, your spleen may be enlarged. This is because in ET your spleen may begin to produce blood cells, and these collect inside the spleen. Spleen enlargement can be checked by feeling your tummy or by an ultrasound or CT scan. The ultrasound is a painless test.
- Bone marrow biopsy (BMB): A bone marrow biopsy is a test of your bone marrow that is done in the hospital. You will not need to stay overnight in the hospital, and you will generally just need local anaesthesia. Your haematologist will give you some medication to prevent pain, and then he or she will extract some bone marrow from your hip bone using a needle. The bone marrow tissue can then be examined in a laboratory so that your haematologist can see how the stem cells in your bone marrow are working, and if there is any fibrosis in your marrow.
Risk levels
If you receive a diagnosis of ET, your haematologist may tell you that you are a low, intermediate or high-risk patient. Risk levels are based on a combination of features including your age and your symptoms especially if you have had a blood clot and perhaps your white cell count. Your haematologist will consider your risk level when making recommendations about your treatment plan.
Treatment
Treatment is a balancing act. Patients and haematologists must work together to judge whether the benefits of treatment outweigh the downsides. The goal of ET treatment is reducing the risk of potential complications while keeping side effects to a minimum.
The first step in any treatment plan is to take good care of yourself. Maintaining a healthy body weight and controlling your blood pressure and cholesterol can go a long way towards protecting your long-term health. It is very important to stop smoking. Your GP or consultant can give you more information on how to best to care for your overall health.
In the early stages of ET you may not have any symptoms and you may be considered low-risk. If this is the case, your haematologist may suggest observation. Observation means that your ET will not be treated with medication (other than possibly low-dose aspirin), but that your medical team will test your blood from time to time for any sign of changes.
ET patients who have intermediate to high-risk have an increased risk of clotting (thrombotic) or bleeding (haemorrhagic) events, so the first goal of treatment is to reduce the likelihood of these events. Haematologists can use a number of different drugs to treat ET. The following treatments are the commonly used to treat ET, read more about them in our Treatment section.
Medications to reduce your risk of clotting
Therapies to reduce your platelet count
- Hydroxycarbamide
- Interferon alpha
- Anagrelide
- Busulphan, melphalan or phosphorous
- Plateletpheresis (removal of platelets)
JAK inhibitors
These are agents currently under intense investigation in this field. Ruxolitinib or Jakavi® was the first to be investigated and much research continues on a regular basis in this area.
Ruxolitinib or Jakavi®
Ruxolitinib blocks the functions of JAK2 and its relation JAK1. This slows down blood cell production, reduces spleen size and symptoms. Jakavi® is only licensed in MF and PV at the present time. It is experimental therapy for ET.
Complications
People with ET are at high risk of blood clots (thrombosis) and bleeding (haemorrhagic) events. Medication can reduce the platelet count, make the platelets less ‘‘sticky’’, and decrease the likelihood of bleeding and clotting complications. Clotting episodes are more common and can be serious. Examples of the different types of blood clots include those listed below. You can read more about preventing and coping with serious clots in our Living with MPNs section.
- Deep vein thrombosis (DVT)
- Pulmonary embolism (lung clot)
- Myocardial infarction (heart attack)
- Cerebrovascular accident (CVA/stroke)
- Minor thrombotic events (minor clots)
- Transient ischaemic attack (TIA/minor stroke)
- Superficial thrombophlebitis (varicose veins)
- Erythromelalgia (painful and swollen finger or toe)
The risk factors for these clotting events include being over sixty years of age, your general health, and whether or not you have experienced a clot in the past. There are many other risk factors for heart attacks and stroke, including:
- High blood pressure
- Cigarette smoking
- Diabetes
- High cholesterol
- A family history of these conditions
- Being overweight
Bleeding complications
Bleeding complications are less common than clots. Bleeding problems are also less likely if your platelet count is lower than 1000 but more than 80 million per millilitre. Bleeding can appear in a variety of forms from easy bruising and nosebleeds to bleeding from the digestive system and sometimes in the brain.
Less common complications
Less common ET complications include a risk of developing acute myeloid leukaemia, (AML) or myelofibrosis (MF). Some of the drugs used to treat ET can slightly increase your risk of developing acute leukaemia. If you have any concerns about your treatment, please discuss this with your consultant.
Prognosis
If you have ET, your prognosis depends on many factors, including your age and whether you have other illnesses or complications.
ET patients who do not suffer from severe thrombotic (clotting) or haemorrhagic (bleeding) complications can probably expect a near-to-normal lifespan.
Some patients with ET develop acute myeloid leukaemia (AML) or myelofibrosis (MF) at a late stage of the illness. When ET ‘‘transforms’’ to leukaemia or myelofibrosis, the outlook can be poor, as these diseases are often resistant to treatment. Your haematologist will monitor your blood and general health regularly. If there are any signs of leukaemia or myelofibrosis, your haematologist will find these and offer the appropriate treatment.
You can learn more about myelofibrosis on our myelofibrosis page. You can learn more about leukaemia by visiting Blood Cancer UK (formerly Bloodwise).
Your Guide to Essential Thrombocythaemia (ET)
Information and advice about causes, symptoms and management. Download a copy of our information booklet here…